Consortium News
Welcome to the TRICIA News Page. Here you’ll find the latest updates from the Tissue Research in Childhood Inflammatory Arthritis (TRICIA) Consortium – including network updates, research discoveries, upcoming events, and stories from families and clinicians involved in our work to improve the future of children and young people with JIA.
Stay Connected with the TRICIA Network!
Be the first to hear about our latest research news. Whether you’re a researcher, clinician, patient partner, or supporter of paediatric rheumatology, sign up to receive updates and be part of the TRICIA community.
We promise not to overload your inbox—and you can unsubscribe at any time. Read the Privacy Notice

Patient and Family Input Shapes Next Stage of MAPJAG Research
Patients, parents and researchers recently came together to help shape the next stage of research building on the MAPJAG study.
We are grateful to those who shared their experiences and perspectives.
Lizzy Rosser from University College London presented early ideas for a new grant application based on findings from the MAPJAG study. The proposed work aims to better understand differences between children with arthritis, with the goal of supporting more targeted treatment approaches.
The session focused on gathering feedback at an early stage, before the proposal is finalised. Participants explored how key concepts are explained, how clinical questions are framed, and what outcomes matter most to families.
A clear message from the discussion was the importance of focusing on impact. Participants emphasised that explanations should link back to how research could improve treatment and outcomes, particularly for those who do not respond to current therapies.
The discussion also highlighted the complexity of lived experience, including variation in age of onset, time to diagnosis and disease subtype. These insights will help refine both the research questions and how the work is communicated.
This input will directly inform the development of the grant application and the wider programme of work. It also shows how findings from MAPJAG are already being used to generate new research questions and shape future studies, including programmes such as ARCADIA.
This reflects the wider aim of the TRICIA network to support research that is both scientifically robust and shaped by patient experience.


MAPJAG Study Reaches 100 Participants
We are pleased to share that the MAPJAG study has now recruited its 100th participant, marking an important milestone in the delivery of tissue-based research in childhood arthritis.
Since opening in 2021, the study has progressed from an initial set-up phase into an active programme, supported by established clinical and laboratory pathways across participating centres. This milestone reflects both that progress and the commitment of the children, young people and families who have taken part so far.
MAPJAG was established to understand what is happening inside the joint by analysing synovial tissue from children and young people with inflammatory arthritis.
Early work focused on developing safe and practical approaches to synovial tissue biopsy in children. This included designing and implementing standard operating procedures for both large and small joint biopsies, alongside protocols for sample collection, processing, storage and transport. These approaches are now embedded in routine study delivery.
In parallel, the study has established a dedicated tissue analysis pipeline, linking clinical data with biological samples and ensuring consistency across sites. Tissue samples are processed locally and transferred for quality control, storage and downstream analysis using standardised methods.
The study has also introduced systems for consistent data capture and management, using a shared dataset and central database to support harmonised data collection and analysis.
Reaching 100 participants demonstrates the feasibility of collecting high-quality synovial tissue samples in children and young people within a multi-centre study.
This milestone comes as the MAPJAG network continues to expand, with new sites preparing to open across the UK and internationally. As these sites begin recruitment, the number and diversity of samples available for analysis will continue to increase.
As the study grows, increasing the number and diversity of samples will strengthen analyses and help accelerate new insights.
Further findings from the study are expected in the coming months, including work exploring the acceptability and tolerability of biopsy procedures in children and young people.
Together, these developments are helping to build a robust platform for tissue-based research in childhood arthritis and support the long-term aim of more targeted and effective treatments.
We are grateful to all the families who have contributed to this milestone.
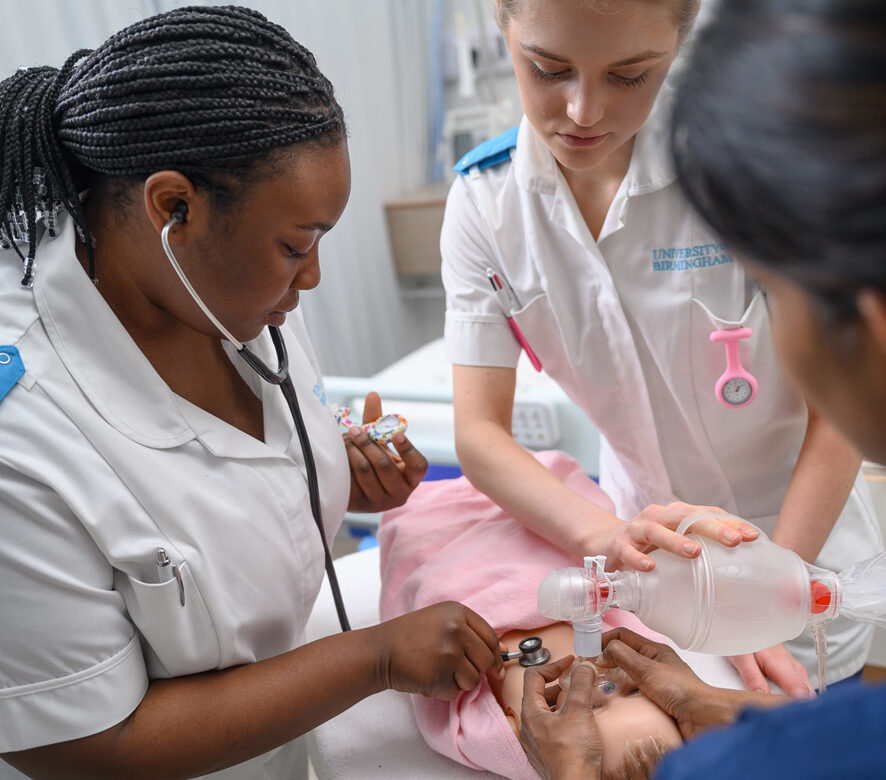
MAPJAG Study Expands to Include Healthy Comparator Group
We are pleased to share that the MAPJAG study has been expanded to include a healthy comparator group, marking an important step forward in our ability to understand childhood arthritis at a tissue level.
MAPJAG focuses on analysing synovial tissue from children and young people with inflammatory arthritis to better understand what is happening inside the joint, where the disease takes place. Until now, this work has focused on characterising disease. Building on the first MAPJAG results published through the TRICIA network, this expansion allows us to place disease findings in the context of healthy joint biology.
The comparator samples are not taken from “healthy volunteers” in the traditional sense. Instead, tissue is collected, with consent, from individuals who are already undergoing clinical procedures where small amounts of tissue would otherwise be discarded. This approach ensures that samples can be obtained in a way that is both ethical and acceptable, without requiring additional invasive procedures.
Why this matters
Including this comparator group will allow us to more clearly distinguish which features are specific to disease and which reflect normal joint biology. This is an important step towards identifying the cellular and molecular changes that drive inflammation, and towards understanding what a truly healthy joint looks like at a tissue level.
This expansion also strengthens the wider research programme, including work within the ARCADIA consortium, where comparing diseased and non-diseased tissue is central to defining remission and predicting relapse.
Although the amendment has now been approved and implemented across sites, sample collection is still in the early stages as we establish the practical pathways required. As this develops, the inclusion of comparator samples will help build a more complete picture of joint biology in children and support the long-term aim of more targeted and effective treatments.
Juvenile idiopathic arthritis research led by TRICIA Network featured in Hospital Healthcare Europe
Research exploring juvenile idiopathic arthritis (JIA) and the biology of the disease has recently been highlighted in a feature published in Hospital Healthcare Europe. The article focuses on work led by Professor Lucy Wedderburn and Professor Adam Croft, who also lead the TRICIA Network, alongside Dr Chrissy Bolton and colleagues.
The feature describes how researchers are studying synovial tissue from the joints of children with JIA to better understand the biological processes driving the disease. Historically, much research into childhood arthritis has relied on blood samples or evidence extrapolated from adult rheumatoid arthritis studies. However, inflammation in JIA occurs primarily in the synovial lining of the joint, meaning that studying this tissue directly provides a much clearer picture of the disease.
Understanding synovial tissue in juvenile idiopathic arthritis
Using advanced imaging and gene profiling technologies, the research team has begun mapping the cellular architecture of the inflamed joint in children. Early findings suggest that the immune cells involved in JIA may vary across different stages of childhood, with younger children and teenagers showing distinct cellular patterns.
These insights could help explain why treatments work differently between patients and may support the development of more personalised approaches to care.
The work highlighted in the article reflects wider collaborative research efforts across the paediatric rheumatology community.
In particular, it builds on research developed through the CLUSTER consortium, funded by the Medical Research Council and Arthritis UK (Versus Arthritis), which brings together researchers across the UK studying juvenile idiopathic arthritis and related conditions such as uveitis.
The article also highlights the many contributors involved in this work, including clinicians, research nurses, interventional radiologists, laboratory scientists and bioinformaticians, as well as the children and families who take part in research studies. The growing visibility of this work reflects increasing international interest in understanding the biology of juvenile idiopathic arthritis through tissue-based research.
You can read the full article in Hospital Healthcare Europe:

New ARCADIA Consortium Builds on MAPJAG to Redefine Remission in Arthritis
The ARCADIA arthritis remission study has been awarded £3 million in funding from Arthritis UK, bringing together leading centres across the UK and Europe to address a key challenge in inflammatory arthritis: how to accurately define when remission has truly been achieved.
Running from November 2025 to October 2030, the ARCADIA consortium will focus on understanding remission at a biological level, with the aim of supporting safer treatment decisions and, ultimately, long-term drug-free remission for people living with arthritis.
Why this research matters
A central strength of the ARCADIA study is its ability to include children and young people alongside adults. This is made possible through the infrastructure developed within the TRICIA network, including the MAPJAG observational study, which has established safe and acceptable approaches to collecting synovial tissue in children, alongside standardised protocols and well-characterised patient cohorts.
Until recently, studies of remission have relied largely on adult data, with limited insight into joint biology in children. MAPJAG has begun to address this gap, enabling ARCADIA to incorporate paediatric tissue data and explore how remission differs across the life course.
At present, remission is assessed using clinical examination and blood tests, which cannot distinguish between true absence of disease and disease that is suppressed but still present. This uncertainty means that many patients experience relapse after stopping treatment.
The ARCADIA arthritis remission study aims to move beyond this by focusing on “tissue remission”, using detailed analysis of joint samples to determine whether the disease has truly resolved.
Building on MAPJAG and TRICIA
ARCADIA builds directly on the foundations laid by MAPJAG and the TRICIA network, extending tissue-based research into a larger, multi-centre programme. By combining data from children and adults, the consortium aims to develop a more accurate and biologically grounded definition of remission.
As more tissue data are generated and analysed, this work will support the development of tools to predict relapse and guide treatment decisions, helping to ensure that the right patients can safely reduce or stop medication at the right time.

Young people share their views on synovial biopsy research
On 7 October 2025, members of the TRICIA Network joined a special Your Rheum session to talk with young people about ultrasound-guided synovial biopsy. Your Rheum is a group for 11-24 year olds across the UK with diagnosed rheumatic conditions, where you can advise, input and shape current adolescent and young adult rheumatology research. Although the procedure has been discussed with children and adults in the past, this was the first time it had been explored specifically with adolescents and young adults.
The online meeting brought together fourteen young people aged 15 to 25 (mostly female), Your Rheum representatives Catherine Wright and Dr Victoria Harbottle, and researchers including Professor Coziana Ciurtin, Professor Adam Croft, Dr Charlene Foley, Dr Christine Bolton and Dr Laura Scagnellato.
Why biopsies are used in JIA research
The discussion was particularly timely because University College London Hospitals (UCLH), led by Professor Ciurtin, is joining the TRICIA Network as a new recruiting site. UCLH’s adolescent clinic will play an important role in offering biopsies to young people with Juvenile Idiopathic Arthritis (JIA), so hearing their views directly was an important step in shaping how the procedure is introduced and explained.
Researchers outlined why biopsies are used in JIA research. Studying the synovial tissue lining the joint, where inflammation occurs, can help scientists understand how the disease develops and how future treatments might be tailored more precisely.
They explained that the minimally invasive procedure is carried out under ultrasound guidance through a small skin entry point. For young people, the biopsy would be performed under local anaesthetic rather than general anaesthetic, and Entonox may also be offered to help with comfort. Importantly, researchers reassured participants that the small piece of tissue collected does not affect normal joint function.
Questions raised by young people
Young people asked practical and thoughtful questions. They wanted to know whether general anaesthesia could ever be used, when steroid injections are given in relation to the biopsy, and whether the procedure would be offered as part of treatment or purely for research.
They also asked how clinicians distinguish between tissue important for joint function and tissue involved in inflammation, and whether biopsies can be performed during remission or only during a flare. Others were interested in what symptoms might occur afterwards and how long the technique has been used in clinical practice.
Poll results from the session
A quick emoji poll gave insight into attitudes towards different types of studies:
- Twelve said they would take part in a biopsy study, with two unsure
- Seven would agree to a biopsy while their arthritis was controlled, three would not, and one was unsure
- Only three would join a drug trial involving biopsies before and after treatment, while eight said no, largely due to concerns about untested drugs
- Seven would join a medication stop study with biopsy, and ten said they would agree to a repeat biopsy after a flare
The discussion suggested that young people see greater value in biopsies when they are linked to a personal clinical decision, such as stopping medication, rather than when they are part of purely observational research. This insight will help shape how research opportunities are presented in adolescent clinics at UCLH and other TRICIA sites.
What information young people want
Participants also shared what information would help them feel more comfortable about the procedure. They wanted to know which joints are suitable for biopsy, whether smaller joints can be sampled, and whether this makes the procedure more difficult. They also asked whether findings from their own biopsy could be shared with them, and raised common anxieties about needles and blood tests.
Several participants suggested that a short video showing each stage of the procedure would be particularly helpful. Seeing what happens step by step, including the sounds, sensations and what to expect afterwards, could help reduce anxiety and make the experience feel more predictable.
Another question touched on how biopsy findings might guide treatment or help predict response to therapy, and whether this could lead to more personalised approaches in the future. Although time ran out before this could be explored in depth, it reflected a strong interest in how tissue research might ultimately improve care.
Shaping how biopsies are introduced
Feedback from this Your Rheum session will directly inform how biopsies are introduced to young people at UCLH. The procedure will be offered under local anaesthetic only, with clear explanations about each stage of the process, including when steroid injections may be given and what sensations to expect.
The TRICIA Network will also work with Your Rheum and other patient partners to co-create short, age-appropriate explainer videos and visual resources showing exactly what happens during the biopsy. These materials will support informed decision-making and help young people feel more confident about what to expect.
The TRICIA team would like to thank the Your Rheum members for their openness, thoughtful questions and constructive feedback. Their input is already shaping how biopsies are discussed with young people and will help ensure that future research reflects their priorities.

Professor Lucy Wedderburn appears on ITV News to discuss MAPJAG study
Professor Lucy Wedderburn, Consultant Paediatric Rheumatologist at Great Ormond Street Hospital (GOSH) and co-lead of the MAPJAG study, appeared on ITV News this month (July 2025) to discuss groundbreaking new research into childhood arthritis.
The segment, which aired nationally, highlighted how the MAPJAG study is helping scientists understand why children respond differently to treatment, and how tissue samples taken during routine procedures could lead to more personalised therapies in the future.
Lucy shared how close collaboration with families and children has been essential in enabling this research to happen safely and ethically. Her appearance also helped shine a light on the often invisible impact of juvenile idiopathic arthritis (JIA) and the need for more child-focused research.

First Results from MAPJAG Published in Science Translational Medicine
The first published results from the MAPJAG study have been released in the prestigious journal Science Translational Medicine, marking an important milestone in understanding childhood arthritis.
In this world-first study, researchers from the University of Birmingham, University College London, Great Ormond Street Hospital and Birmingham Women’s and Children’s Hospital have used cutting-edge technology to analyse synovial tissue biopsies from children with Juvenile Idiopathic Arthritis (JIA), providing unprecedented insights into the cellular changes happening inside the joints of children with arthritis.
Why this matters
Juvenile idiopathic arthritis affects over 10,000 children in the UK, causing long-term pain, joint damage and disability. Treatments are available but are often based on a trial-and-error approach, as children respond differently to medications. This new research is a major step towards understanding why treatments work differently in different children.
Groundbreaking discoveries from the first phase of MAPJAG:
- First high-resolution “map” of inflamed joint tissue in children with arthritis.
- Identification of unique cellular fingerprints linked to disease severity and age.
- Clear differences were found between children and adults, explaining why children need age-specific treatment strategies.
- The study confirms that tissue analysis can provide insights that blood tests alone cannot.
- These early findings lay the groundwork for future precision medicine approaches, aiming to match the right treatment to each child.

Mapping out the networks of cells in the joint reveals a pink barrier layer, navy immune cells flooding in through light blue blood vessels, which increase in number as the disease continues
“We know how frustrating it can be for families and young people to find a drug that best works for their arthritis. Finding ways to better predict which medicines will be beneficial for a particular child would mean we were able to treat the disease more rapidly and effectively. To achieve this goal, we first needed to understand what cells make-up the lining of the joint where the inflammation occurs. Equipped with that knowledge, we can now start to tackle the next challenge, determining how these cellular fingerprints within the joint tissue can help us predict which drug will work best, ensuring we give the right drug, to the right child, at the right stage of their disease.”
Professor Adam Croft, Chief Investigator of the study
“This study represents a real step change in our work with children and young people who live with arthritis, and has been a huge team effort. Rather than having to rely on blood tests which often do not tell us accurately what is happening in the joint, we can now directly analyse the joint lining, across different types of childhood arthritis and different ages. Our findings show that younger children have different types of immune cells invading their joints compared to older children. Samples from children with arthritis looked different to adult samples, with a different make up of immune cells, blood vessels and distinct connective tissue cells. This suggests that treatments may need to vary depending on age and shows why we can’t just extend studies from adult studies to understand arthritis in children.”
Professor Lucy Wedderburn, Co-Lead Investigator
Read the full paper:
These are preliminary results from the first 19 participants, with many more samples already collected. The MAPJAG study continues to grow, with more exciting results to come as additional tissue samples are analysed. This research is helping lay the foundation for precision medicine in childhood arthritis, ensuring every child has the best chance of early, effective treatment.
>> ⬇️ Download full press release here (PDF) <<
>> 🎥 Watch coverage from ITV News here (Opens new page) <<
>> ⬇️ Download the lay summary here (PDF) <<
The lay summary explains the research and its findings in everyday language for patients, families, and the wider public. It was developed in collaboration with our patient and parent involvement (PPI) members, helping to ensure the content is accessible to families affected by childhood arthritis.

Prestigious EULAR Award for Dr Chrissy Bolton
We were delighted to share that Dr Chrissy Bolton received the prestigious 2025 Basic and Translational Science Prize from the European Alliance of Associations for Rheumatology (EULAR).
The EULAR Basic and Translational Science Award was one of the most sought-after honours at the EULAR Congress, recognising the most outstanding scientific abstracts in basic and translational research. This highly competitive award was selected from thousands of submissions and celebrated work that advanced understanding of disease mechanisms and translated scientific discoveries into meaningful clinical impact.
Dr Bolton presented her research, titled “A multimodal dissection of spatial tissue niches associated with severity in childhood arthritis”, in the cutting-edge session on “Omics and New Targets in Spondyloarthropathy and Other Inflammatory Arthritis”.
Her award-winning research focused on studying childhood arthritis, known as juvenile idiopathic arthritis (JIA), by examining joint tissue at a remarkably detailed level. The project aimed to uncover how interactions between different cell types in the joint lining worsened disease severity, with the goal of improving treatment choices for children through a more precise understanding of their disease.
The EULAR 2025 Congress took place in Barcelona, Spain, from 11 to 14 June at the Fira de Barcelona conference centre. The event brought together over 14,000 participants from across the world, including researchers, clinicians, and industry leaders, to share the latest scientific and clinical advances in rheumatology.
Dr Bolton’s award highlighted the remarkable progress of the research team in overcoming long-standing challenges in tissue-based studies of childhood arthritis, made possible through technological advances and collaborative effort. It also reflected the growing recognition of the importance of understanding disease mechanisms in children to improve long-term outcomes.

Dr Chrissy Bolton is a paediatric doctor and MRC Clinical Research Training Fellow undertaking her DPhil at the University of Oxford (Kennedy Institute) and is jointly supervised by Professor Adam Croft at the University of Birmingham. She is a co-investigator in the MAPJAG observational study. You can read more about Chrissy’s recent work in Science Translational Medicine (Vol 17, Issue 805) in our news section.
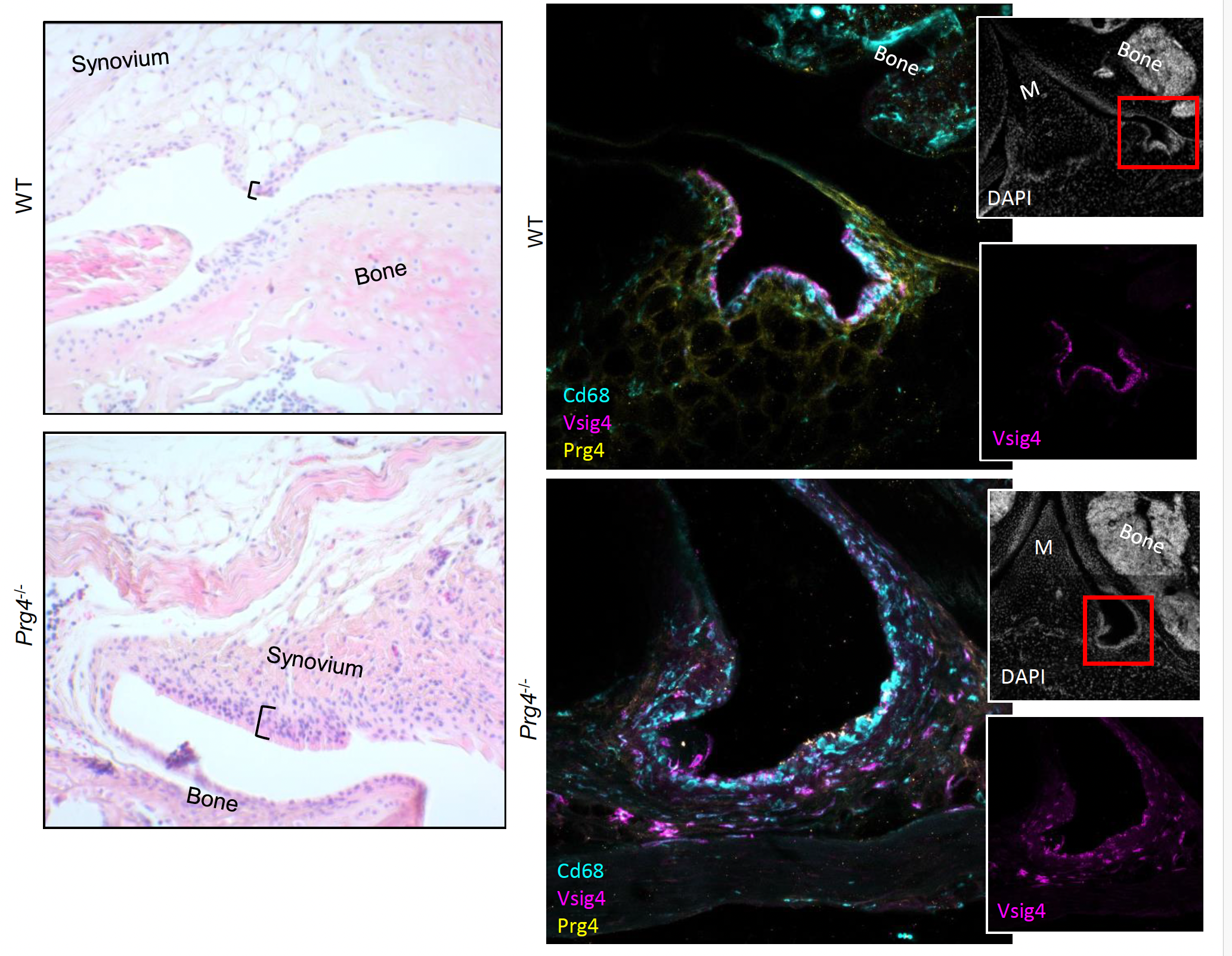
Defining Cellular Pathology in CACP Syndrome: A New Research Initiative
Exciting New Funding Award to Tackle Rare Childhood Arthritis Syndrome
Professor Adam Croft has received funding from Great Ormond Street Hospital Charity for a 3-year research project to study a rare genetic condition called Camptodactyly-Arthropathy-Coxa Vara-Pericarditis (CACP) syndrome.
This debilitating condition begins in early childhood, causing joint stiffness, swelling, and difficulty moving. It can also lead to fluid around the heart (pericarditis), impacting children’s daily lives. Currently, there is no cure or specific treatment.
Understanding the Cause
CACP syndrome is caused by changes in a gene called PRG4, which produces a protein called lubricin. Lubricin helps protect and lubricate joints. Without it, children experience painful joint damage and scarring. However, researchers still don’t fully understand why the lack of lubricin causes these symptoms.
This project will investigate how cells in the joint, called fibroblasts and macrophages, normally work together to keep joints healthy, and what goes wrong when lubricin is missing. The research team believes that without lubricin, macrophages can’t function properly, leading to overactive fibroblasts, inflammation, and scar tissue formation.
Who’s Involved?
Led by Prof. Croft at the University of Birmingham, the study brings together a team of experts from Birmingham Children’s Hospital and the UCL Great Ormond Street Institute of Child Health. It also uses precious joint tissue samples already collected through the UK-wide TRICIA (Tissue Research in Childhood Inflammatory Arthritis) network.
Guided by the Voices of Patients and Families
A unique feature of this study is how closely it has been co-developed with young people affected by CACP and their families. Through a series of meetings in spring 2024, young people (aged 13–21) and their parents shaped the study’s direction. Their experiences highlighted the urgent need to understand and treat joint contractures, which most impact daily life.
They also helped researchers decide when and how to collect tissue samples in an ethical and acceptable way, such as during clinical procedures already being done for care.
Families stressed the importance of new treatments and shared their views on side effects, educational impact, and participation in sports. Based on their input, the study now includes a dedicated work package focused on restoring lubricin and testing potential new therapies.
A National Research Effort
The project is part of the MRC-funded TRICIA consortium, which builds capacity for joint tissue research in children and young people across the UK. Samples used in this study were collected through MAPJAG, a TRICIA-linked study using safe, ultrasound-guided biopsies.
Ongoing Involvement and Communication
Three young people with CACP and their families will remain involved through a study advisory group, meeting regularly to guide research and ensure results are shared clearly and accessibly.
Dissemination will include lay summaries, social media updates, press releases, and public events. The study also contributes to training future scientists through the Patient Alliance initiative, where researchers are paired with PRPs to promote meaningful involvement throughout.

New Video – Amy’s Experience of Living with JIA
At the end of last year the MAPJAG research team collaborated with Amy, a young person living with Juvenile Idiopathic Arthritis (JIA), to create a new video highlighting the importance of research into the condition.
Showcasing the Patient Perspective The video, featuring Amy and Professor Adam Croft, Chief Investigator of MAPJAG, sheds light on the challenges of living with JIA and the vital role research plays in improving treatments. Amy shares her personal journey, including her diagnosis at age three, her experiences with different treatments, and how research has helped shape better understanding and care for young people like her. Professor Croft explains:“Through MAPJAG, we aim to better understand JIA and improve treatments for young people. Collaborating with Amy on this video has been invaluable in showing why research matters—not just to scientists and clinicians, but to the young people affected by this condition every day.”You can watch the video here: https://youtu.be/oXUB-dL2r_4. A Platform for Young Voices in Research Amy’s involvement in this video highlights the importance of patient engagement in research. By sharing her lived experience, she provides a powerful perspective on why studies like MAPJAG are essential for identifying better treatments and ensuring that young people receive the right support as early as possible. Amy reflects:
“It’s important that research focuses on the needs of young people with JIA. Being part of this video was a great opportunity to share my experience and to help raise awareness of the work being done to improve treatment options.”Expanding the Impact of MAPJAG The MAPJAG study continues to grow, supported by funding from the Kennedy Trust for Rheumatology Research, Versus Arthritis, the NIHR Birmingham Biomedical Research Centre, and the Medical Research Council, and remains committed to working closely with young people and their families. Through initiatives like this video, the research team hopes to increase awareness, encourage participation, and ensure that young voices remain at the heart of scientific progress.
New Video – The Importance of Research into JIA
Sharing the Patient Perspective
Two young people, Jasmine and Sophie, who both live with Juvenile Idiopathic Arthritis (JIA), have created a powerful video explaining why research into the condition is so important. As Patient Partner Group members, they contribute invaluable insights and feedback to the TRICIA network, ensuring that research reflects the real concerns of those living with JIA.
Why Research Matters
In the video, Jasmine and Sophie share their personal experiences with JIA, the challenges they face, and how research can improve treatment options. Their voices bring a unique and powerful perspective, helping researchers, funders, and other stakeholders understand the impact of JIA and the need for continued investment in research.
A Valuable Resource for Advocacy
The video serves as an impactful resource for presentations to funders, researchers, and healthcare professionals. Hearing directly from those affected by JIA reinforces the urgency of research and the real-life difference it makes. No one can articulate the need for progress better than those living with the condition.
Watch the Video
You can watch Jasmine and Sophie’s video here: https://www.youtube.com/watch?v=Io10pTLQlXY&t=21s
Produced in March 2024, this video is a testament to the importance of patient involvement in shaping research and driving meaningful change.

Nature Publication success for Chrissy Bolton
Congratulations to Dr. Chrissy Bolton, an MRC Clinical Research Training Fellow and paediatric doctor, on her recent publication in Nature Reviews Rheumatology titled “All fibroblasts are equal, but some are more equal than others.”
Dr. Bolton graduated from the University of Cambridge and UCL, earning national and university prizes in Paediatric Health, Endocrinology, Pain Medicine, Cardiology, and Ethics. She has contributed to pioneering studies on minimally invasive tissue biopsies in children with arthritis, collaborating with Professors Lucy Wedderburn and Adam Croft. Her research focuses on understanding inflammation persistence in juvenile idiopathic arthritis (JIA).
In her recent article, Dr. Bolton explores how epigenetic programming of synovial fibroblasts—the cells lining the joints—affects their response to inflammation. This research sheds light on why different joints may exhibit varying patterns of involvement and responses to treatment in arthritis.
This insight is significant for TRICIA’s mission to integrate synovial tissue analysis into clinical practice for JIA. Understanding the diverse behaviours of synovial fibroblasts can lead to more targeted and effective treatments for young patients with arthritis.
Read the full article >> Bolton, C., Croft, A.P. All fibroblasts are equal, but some are more equal than others. Nat Rev Rheumatol (2024). https://doi.org/10.1038/s41584-024-01097-6

Professor Adam Croft inaugural lecture: Restoring order to the joint: fibroblasts as cellular checkpoints of inflammation
On 6 March 2024, Professor Adam Croft, the Versus Arthritis Chair of Rheumatology and Head of the Rheumatology Research Group at the University of Birmingham, delivered his inaugural lecture titled “Restoring Order to the Joint: Fibroblasts as Cellular Checkpoints of Inflammation.”
In his lecture, Professor Croft explored the critical role of fibroblasts—structural cells within joint tissues—in orchestrating inflammation in chronic joint diseases such as rheumatoid arthritis. He described fibroblasts as the “conductors of the immunological orchestra,” highlighting their ability to either amplify or suppress inflammatory responses. His research has identified distinct fibroblast subtypes with specific functions: some contribute to joint damage, while others help regulate and resolve inflammation. This understanding paves the way for developing targeted therapies aimed at restoring joint health by modulating fibroblast activity.
The lecture was accessible both in person and online via Zoom, reflecting the university’s commitment to sharing knowledge widely. For those interested in a concise overview of Professor Croft’s insights, the University of Birmingham’s Marketing and Communications Team produced a video ahead of the lecture, available here: https://youtu.be/7pwe0jEzH2Q
Dr Chrissy Bolton – Runner-up in the GOSH Image Competition
Dr Chrissy Bolton, MRC Clinical Research Training Fellow and a valued member of the TRICIA team, was recently recognised as a runner-up in a prestigious research image competition. The competition, open to staff from Great Ormond Street Hospital (GOSH) and its affiliated institutes—the NIHR GOSH Biomedical Research Centre (BRC) and the UCL Great Ormond Street Institute of Child Health (UCL GOS ICH)—invited researchers to capture ‘a moment of discovery’ in their work.
This initiative also extended to other paediatric hospitals across the UK, including Alder Hey, Birmingham, and Sheffield, as part of the NIHR GOSH BRC Paediatric Excellence Initiative. From numerous entries, 11 shortlisted images and GIFs were reviewed by three independent panels: the GOSH Young People’s Advisory Group for Research (YPAG), NIHR GOSH BRC stakeholders, and GOSH staff networks. These images highlighted the groundbreaking research conducted across GOSH and its partner institutions, all striving to improve treatments for rare and complex childhood conditions.
Finalists were selected based on their impact and scientific significance, with the overall winner decided through a public vote on social media.

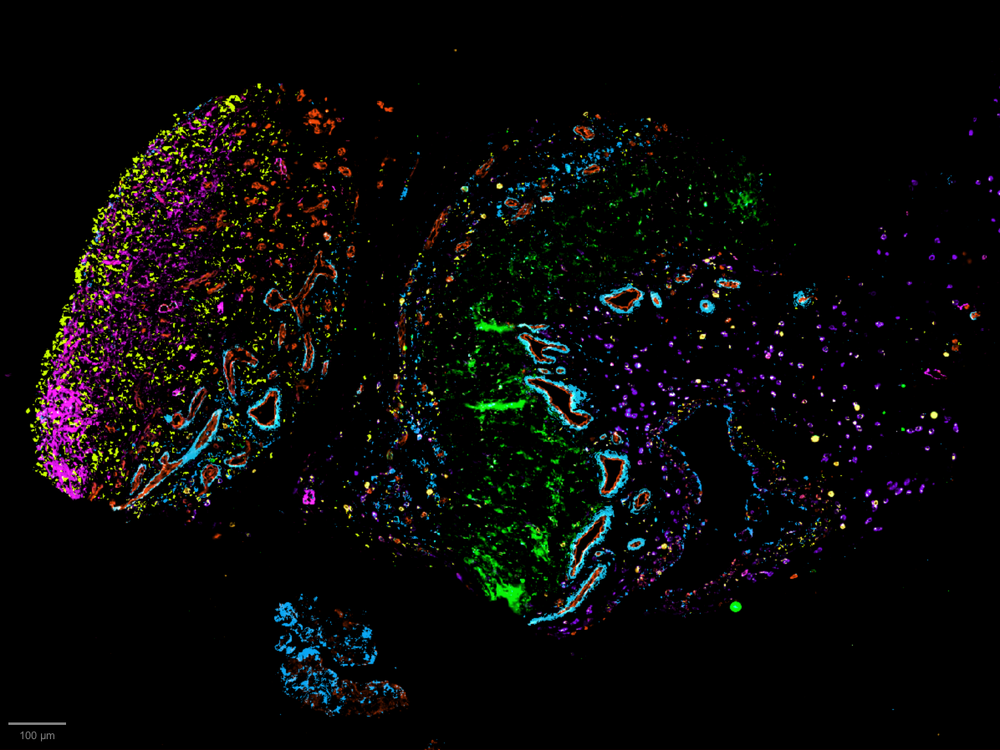
Capturing Childhood Arthritis: Chrissy Bolton’s Image
Dr Bolton’s submitted image provides a striking visual of the cellular landscape within the knee joint of a four-year-old child with arthritis.
• Blood vessels, shown in red, infiltrate the inflamed joint, signalling disease progression and attracting immune cells that drive tissue damage.
• The outer layers, depicted in yellow and pink, typically form a thin protective barrier but thicken as the joint reacts to ongoing inflammation.
• The green regions represent scar tissue, which contributes to joint stiffness and restricted movement.
In the UK, inflammatory arthritis affects approximately 1 in 1,000 children, most commonly impacting large jointssuch as the knees. Despite advancements in treatment, many children continue to experience persistent disease activity for over a decade. Historically, most arthritis research has focused on adults, leaving significant gaps in our understanding of how chronic inflammation develops in children’s immune systems.
This image serves as a powerful reminder of why paediatric-specific research is essential. Parents have been key advocates, demanding that their children benefit from the same cutting-edge scientific advancements as adults. Their voices underscore the urgent need for more research into childhood arthritis, ensuring better treatments and improved outcomes for young patients.

Emerging Investigator Excellence Awards by the American College of Rheumatology
Two researchers from the Institute of Inflammation and Ageing at the University of Birmingham, both affiliated with Professor Adam Croft’s research group and the TRICIA consortium, have been recognised with prestigious Emerging Investigator Excellence Awards by the American College of Rheumatology (ACR).
Dr Chris Mahony and Dr Sam Kemble received these competitive awards for their outstanding contributions to rheumatology research. The Emerging Investigator Excellence Awards acknowledge exceptional abstracts presented by early career researchers, with only one award granted per abstract category.
Dr Chris Mahony: Mapping the Inflamed Synovium in Childhood Arthritis
Dr Chris Mahony, a Postdoctoral Researcher, was recognised in the Paediatric Rheumatology – Basic Science category for his groundbreaking work on juvenile idiopathic arthritis (JIA). His research, titled:
🧬 “Cellular Deconstruction of Stromal and Myeloid Cell Compartments in the Inflamed Synovium of Juvenile Idiopathic Arthritis”,
has led to the creation of the first-ever atlas of the inflamed synovium in children with JIA. This landmark studyprovides new insights into the cellular mechanisms driving inflammation in JIA, paving the way for more effective, targeted treatments for children affected by the disease.
Dr Mahony’s research was made possible through funding from Versus Arthritis, the Kennedy Trust for Rheumatology Research, and the Medical Research Council (MRC).
Dr Sam Kemble: Engineering T Cells to Target Fibroblasts in Inflammatory Disease
Dr Sam Kemble, a Research Fellow, was recognised in the T Cell Biology & Targets in Autoimmune & Inflammatory Disease category for his innovative work on the role of fibroblasts in chronic inflammation. His research, titled:
🧬 “Targeting Fibroblasts in Inflammatory Disease using Engineered T Cells”,
focuses on how tissue-resident fibroblasts contribute to persistent inflammation in diseases such as rheumatoid arthritis (RA) and primary Sjögren’s syndrome (PSS). His team has identified pathogenic fibroblasts in multiple inflammatory conditions and is currently investigating the use of chimeric antigen receptor (CAR) T cells as a novel immunotherapy to specifically target and eliminate these disease-driving cells. This research could lead to a major breakthrough in fibroblast-targeted therapies for inflammatory diseases.
Celebrating Excellence at ACR Convergence 2023
The awards were presented at the ACR Convergence 2023, held at the San Diego Convention Centre, California, from 10–15 November 2023. This flagship annual meeting brings together leading scientists, clinicians, and health professionals from around the world to discuss the latest advancements in arthritis, rheumatic, and musculoskeletal disease research.
Dr Mahony and Dr Kemble’s remarkable achievements reflect the strength of UK-based research in inflammatory diseases and reinforce the University of Birmingham’s role as a leader in rheumatology research. Their work continues to push the boundaries of understanding how inflammation develops and persists, ultimately driving new and more effective treatments for patients.

